Primarily, the tonsil consists of (a) surface epithelium
which is continuous with the oropharyngeal lining; (b)
crypts which are tu be- like invaginations from the surface
epithelium; and (c) the lymphoid tissue. Acute infections
of tonsil may involve these components and are
thus classified as:
1. Acute catarrhal or superficial tonsillitis. Here tonsillitis
is a part of generalised pharyngitis and is mostly seen
in viral infections.
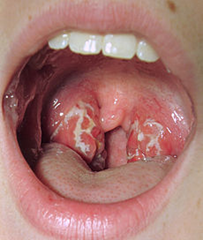
2. Acute follicular tonsillitis. Infection spreads into the
crypts which become filled with purulent material,
presenting at the openings of crypts as yellowish
spots.
3. Acute parenchymatous tonsillitis. Here tonsil substance
is affected. Tonsil is uniformly enlarged and red.
4. Acute membranous tonsillitis. It is a stage ahead of
acute follicular tonsillitis when exudation from the
crypts coalesces to form a membrane on the surface
of tonsil.
Aetiology:
Acute tonsillitis often affects school-going children, but
also affects adults. It is rare in infants and in persons who
a re above 50 years of age .
Haemolytic streptococcus is the most commonly infecting
organism. Other causes of infect ion may be staphylococci,
pneumococci or H. influenzae. These bacteria may primarily
infect the tonsil or may be secondary to a viral
infection.
Symptoms:
The symptoms vary with severity of infection. The predominant
symptoms are:
1. Sore throat.
2. Difficulty in swallowing. The child may refuse to eat
anything due to local pain.
3. Fever. It may vary from 38 to 40°C and may be associated
with chills and rigors. Sometimes, a child
presents with an unexplained fever and it is only on
examination that an acute tonsillitis is discovered.
4. Earache. It is either referred pain from the tonsil or
the result of acute otitis media which may occur as a
complication.
5. Constitutional symptoms. They are usually more
marked than seen in simple pharyngitis and may
include headache, general body aches, malaise and
constipation. There may be abdominal pain due to
mesenteric lymphadenitis simulating a clinical picture
of acute appendicitis.
Signs:
1. Often the breath is foetid and tongue is coasted.
2. There is hyperaemia of pillars, soft palate and uvula.
3. Tonsils are red and swollen with yellowish spots of
purulent material presenting at the opening of
crypts (acute follicular tonsillitis) or there may be a
whitish membrane on the medial surface of tonsil
which can be easily wiped away with a swab (acute
membranous tonsillitis). The tonsils may be enlarged
and congested so much so that they almost meet in
the midline along with some oedema of the uvula
and soft palate (acute parenchymatous tonsillitis).
4. The jugulodigastric lymph nodes are enlarged and
tender.
Treatment:
1. Patient is put to bed and encouraged to take plenty of
fluids.
2. Analgesics (aspirin or paracetamol) are given according
to the age of the patient to relieve local pain and
bring down the fever.
3. Antimicrobial therapy. Most of the infections are due
to streptococcus, and penicillin is the drug of choice.
Patients allergic to penicillin can be treated with
erythromycin. Antibiotics should be continued for
7-10 days.
Complications:
1. Chronic tonsillitis with recurrent acute attacks. This is
due to incomplete resolution of acute infection.
Chronic infection may persist in lymphoid follicles
of the tonsil in the form of microabscesses.
2. Peritonsillar abscess .
3. Parapharyngeal abscess.
4. Cervical abscess due to suppuration of jugulodigastric
lymph nodes.
5. Acute otitis media. Recurrent attacks of acute otitis
media may coincide with recurrent tonsillitis.
6. Rheumatic fever. Often seen in associa tion with tonsillitis
due to Group A beta-haemolytic streptococci.
7. Acute glomerulonephritis. Rare these days.
8. Subacute hacterial endocarditis. Acute tonsillitis in a
patient with valvular heart disease may be complicated
by endocarditis. It is usually due to Streptococcus
viridans infection.
Thank you for sharing this...I am patient of this. in a year I am suffer with it like 3-4 times, any permanent solution for this ?
ReplyDeleteThanks,
Sagar Vyas
You can have your tonsils removed
DeleteThis comment has been removed by the author.
ReplyDeleteSurgical excision-- TONSILLECTOMY, by an ENT specialist.
ReplyDeleteThanks for sharing. Great info.
ReplyDeletePlease I need someone to assure me. My 2 years old girl is having recurrent follicular tonsillitis by a rate every 2 months, our ENT doctor wants a tonsillectomy now at this age. Is it safe or better to wait ?
ReplyDeletePlease I need an answer ASAP
Are you serious blogger. You just copy pasted it from DISEASES OF EAR NOSE AND THROAT by Dr.Dhingra
ReplyDelete@raja bhagat . atleast his case picture is not from dhingra... pictures in that book are awful...
ReplyDeleteNice post!! I would like to thanks for your post, Hearing Loss makes one disconnect from all communication. It effects everyday life. Give Our expert team are here to help you Hear Life again!
ReplyDeleteBest Hearing Hospital in Bangalore | Top Hearing Specialist in Bangalore | Best Hearing Specialist in Bangalore
I got more information about tonsillitis. I feel better after getting treatment by Dr. Pawan Singhal. I would like to suggest for better treatment in jaipur.
ReplyDeleteENT Doctor in Jaipur
Really nice content ... Admin... Have great information I contribute with your experienced... I hope you post again soon. I am very happy to leave a comment for this blog, which really put honest information...
ReplyDeletebest dystonia doctors
cervical dystonia and parkinson's disease
cervical dystonia causes
cervical dystonia cure
cervical dystonia exercises
cervical dystonia medications
I red your blog, you have provide different signs and symptoms of ENT is very informative.Few days back i went to sriramachandra for ENT (Ear, Nose and Throat) checking , the way he care and service is nice.
ReplyDeletehearbal
ReplyDeleteI like it when folks come together and share views. Great blog, keep it up! https://godocweb.com/
ReplyDeleteThis is very educational content and written well for a change. It's nice to see that some people still understand how to write a quality post.! health practicioner
ReplyDeletebiaya konsultasi online covid via whatsapp Thanks for a very interesting blog. What else may I get that kind of info written in such a perfect approach? I’ve a undertaking that I am simply now operating on, and I have been at the look out for such info.
ReplyDelete